Conversational AI
Just Ask. Benvisio Does the Rest.
No complex dashboards to learn. Ask a question in plain English and get rich, visual answers with actionable next steps.

Benvisio gives brokers and HR leaders unprecedented visibility into health plan performance, cost drivers, and optimization opportunities — powered by conversational AI.
The Challenge
US employer health benefits is the largest private insurance market on earth — and one of the least transparent.
Carriers set rates with little transparency. Employers can't tell if they're overpaying by 5% or 25%.
Average renewal increases of 8-12% — far outpacing wages. Budgets strained with no clear path to optimize.
Brokers juggle dozens of carrier quotes in Excel. Apples-to-oranges comparisons miss the best options.
HR leaders make million-dollar decisions without claims analytics, network analysis, or employee impact data.
Conversational AI
No complex dashboards to learn. Ask a question in plain English and get rich, visual answers with actionable next steps.

See It In Action
Rich visual reports and interactive analysis tools — designed for fast, confident decision-making.
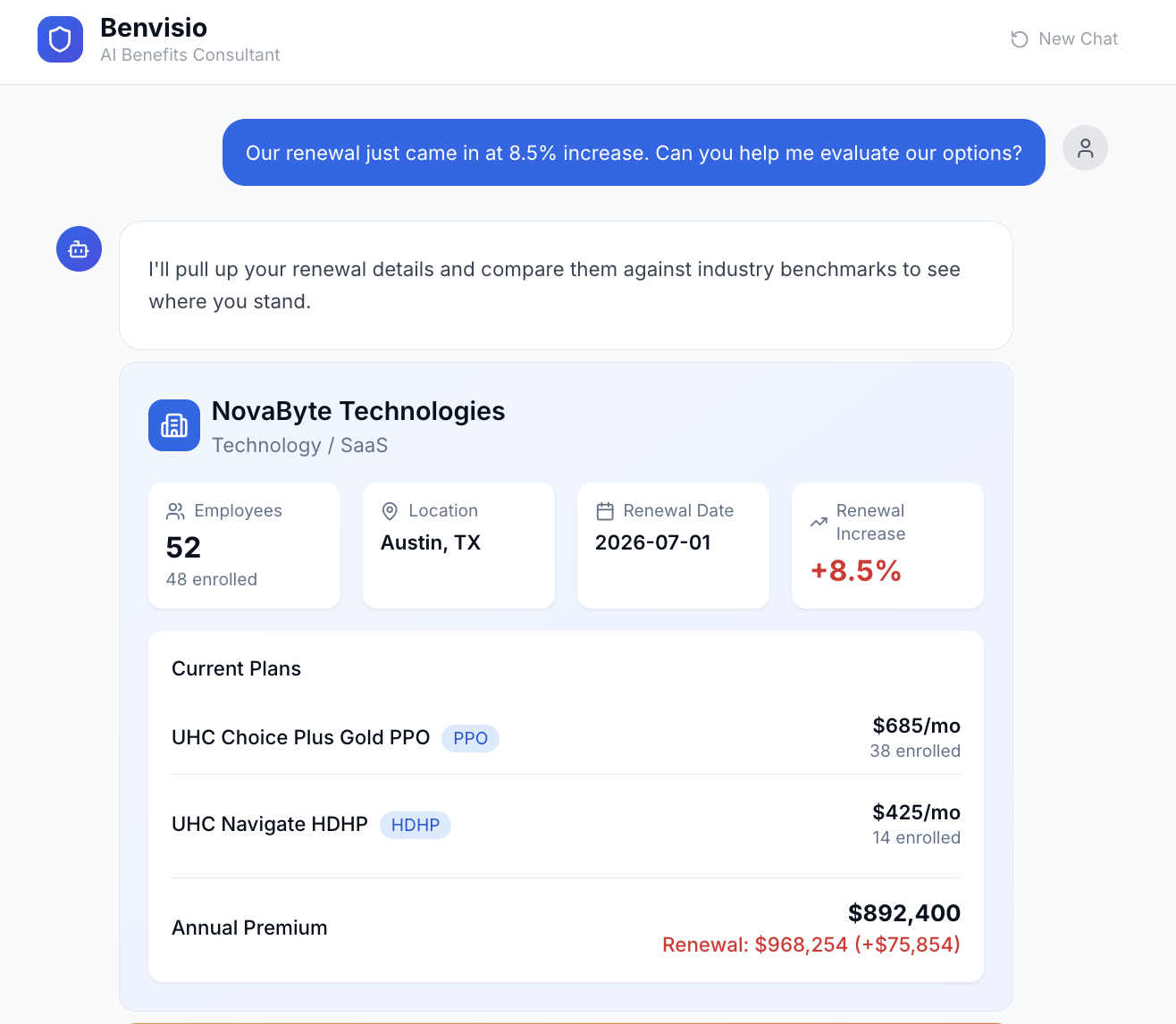
See the complete picture in seconds: current plans, enrollment, premiums, renewal increase, and census demographics — all in one rich visual card.
For Benefits Consultants
Serve more clients, deliver better outcomes, grow your book of business.
Compare plans across every carrier, every funding strategy, every plan design in seconds. No more manual spreadsheet comparisons.
Our AI analyzes claims data, census demographics, network adequacy, and market benchmarks to surface the optimal strategy for each client.
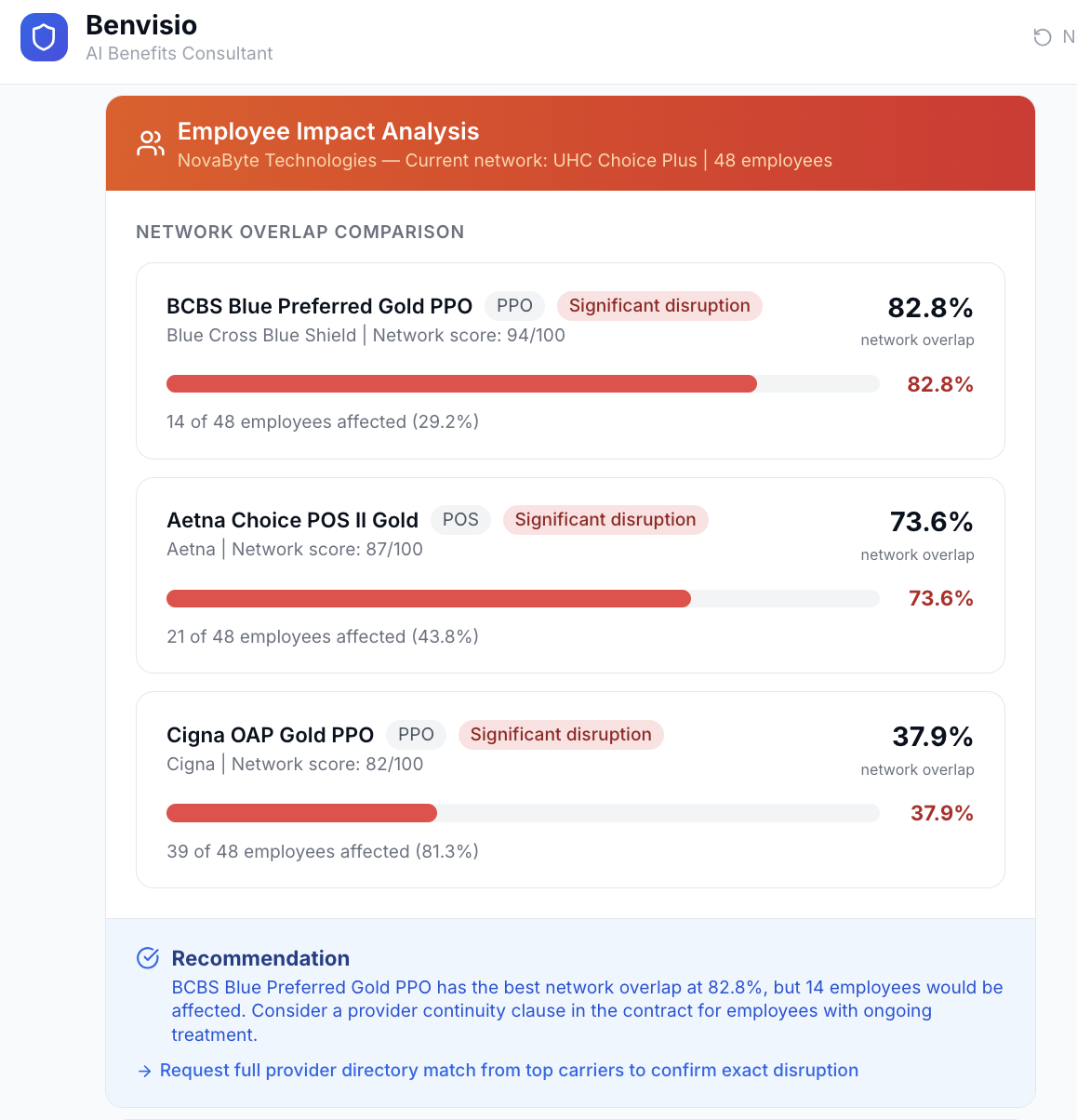
Before recommending a plan switch, see exactly which employees' doctors would be affected. Network overlap %, disruption risk, transition recommendations.
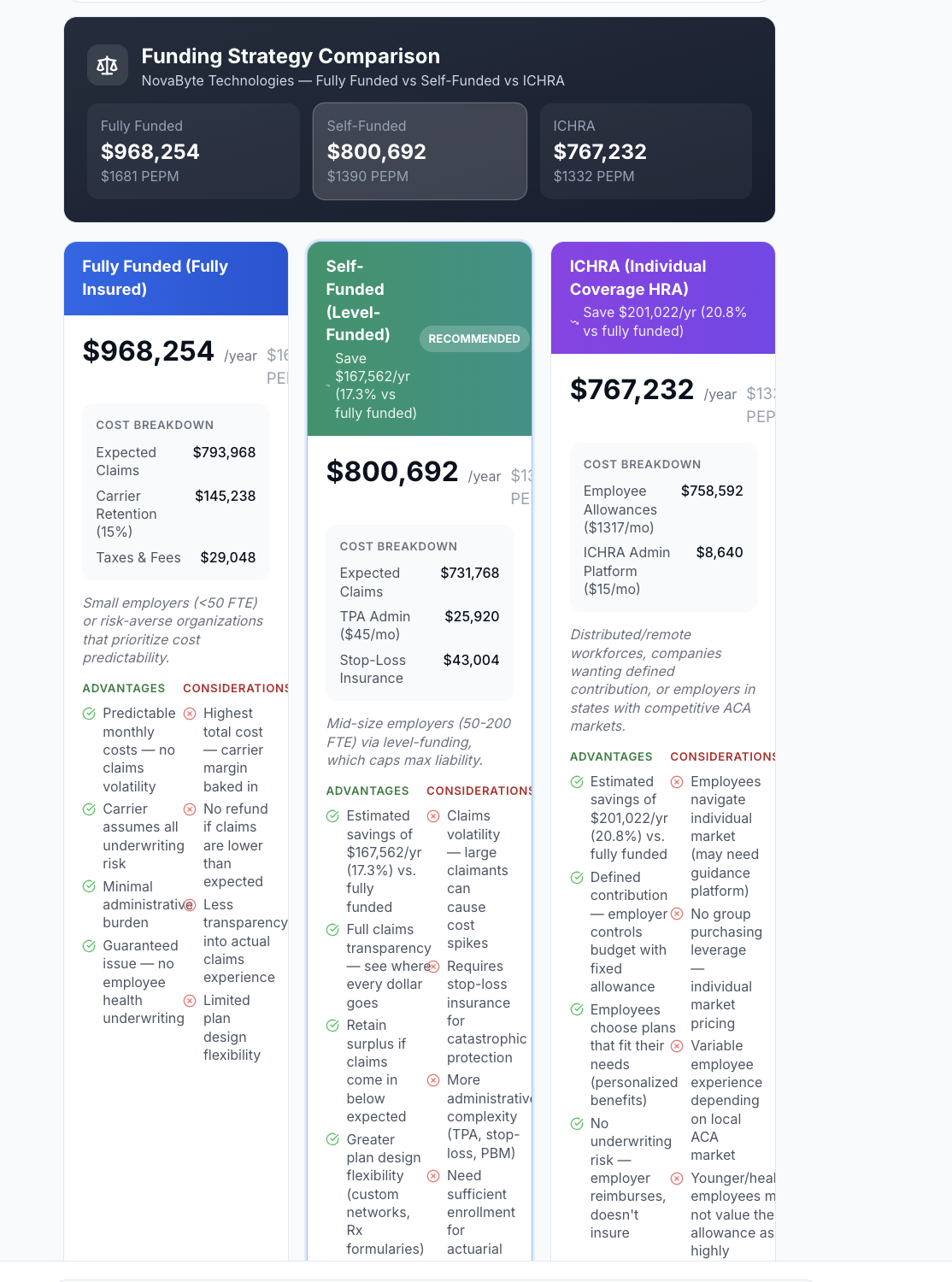
Fully funded vs. self-funded vs. level-funded vs. ICHRA — side-by-side with real cost projections, risk analysis, and tailored pros/cons.
ACA affordability, ERISA requirements, CAA disclosure rules — automatically checked and flagged. Never miss a regulatory requirement.
What used to take days of analysis now takes minutes. Serve more clients without sacrificing quality. Your expertise + our AI = unbeatable.
“Benvisio cut my renewal analysis time from 3 days to 30 minutes. I’ve doubled my book of business while delivering better outcomes for every client.”
For HR & Benefits Leaders
Finally understand where every dollar goes — and how to optimize it.
See your complete benefits landscape in one place: medical, dental, vision, life, disability, stop-loss. Know exactly what you're paying and why.

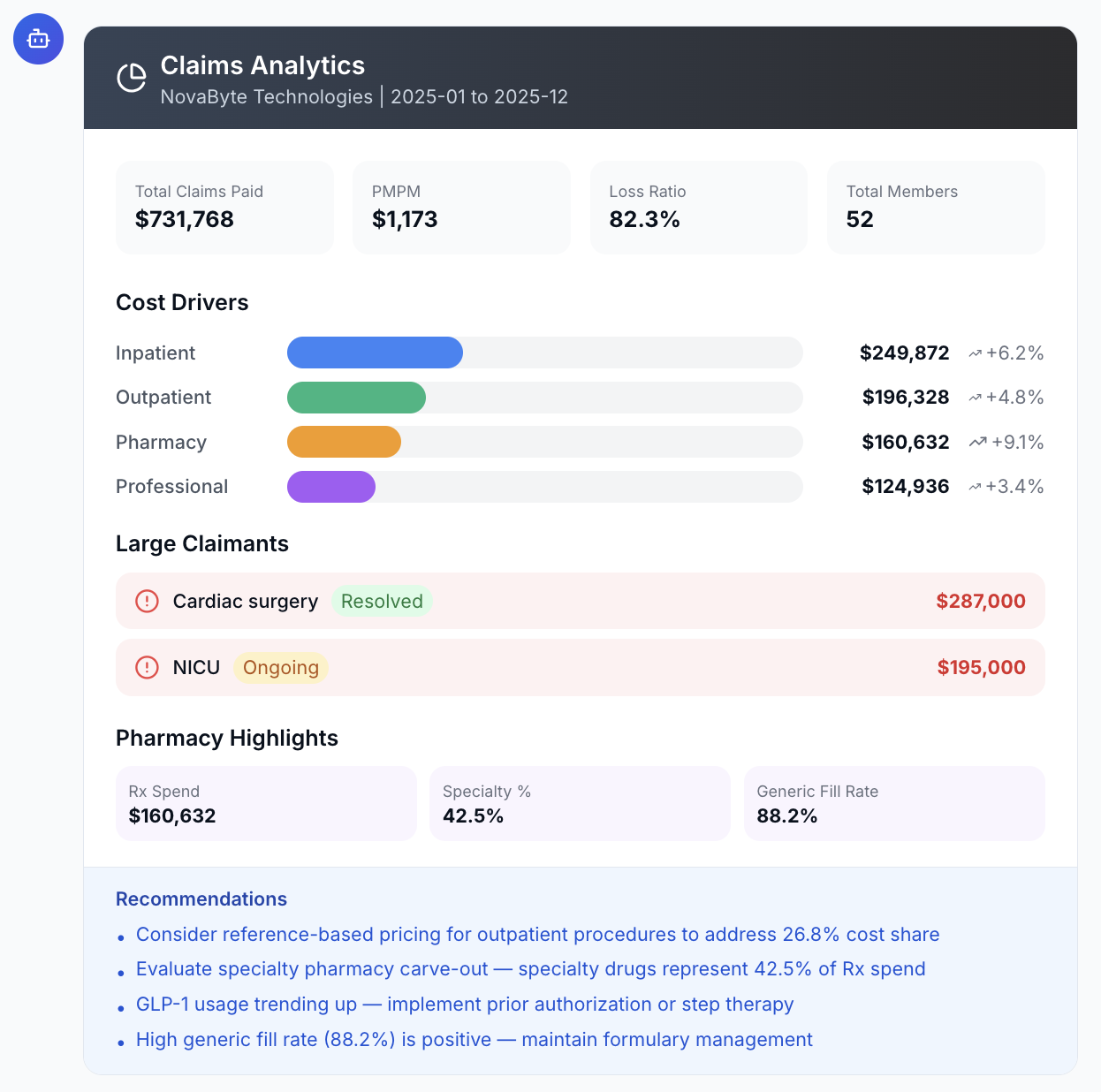
Understand what's driving your costs: inpatient vs outpatient vs pharmacy, large claimants, specialty drug trends — with actionable recommendations.
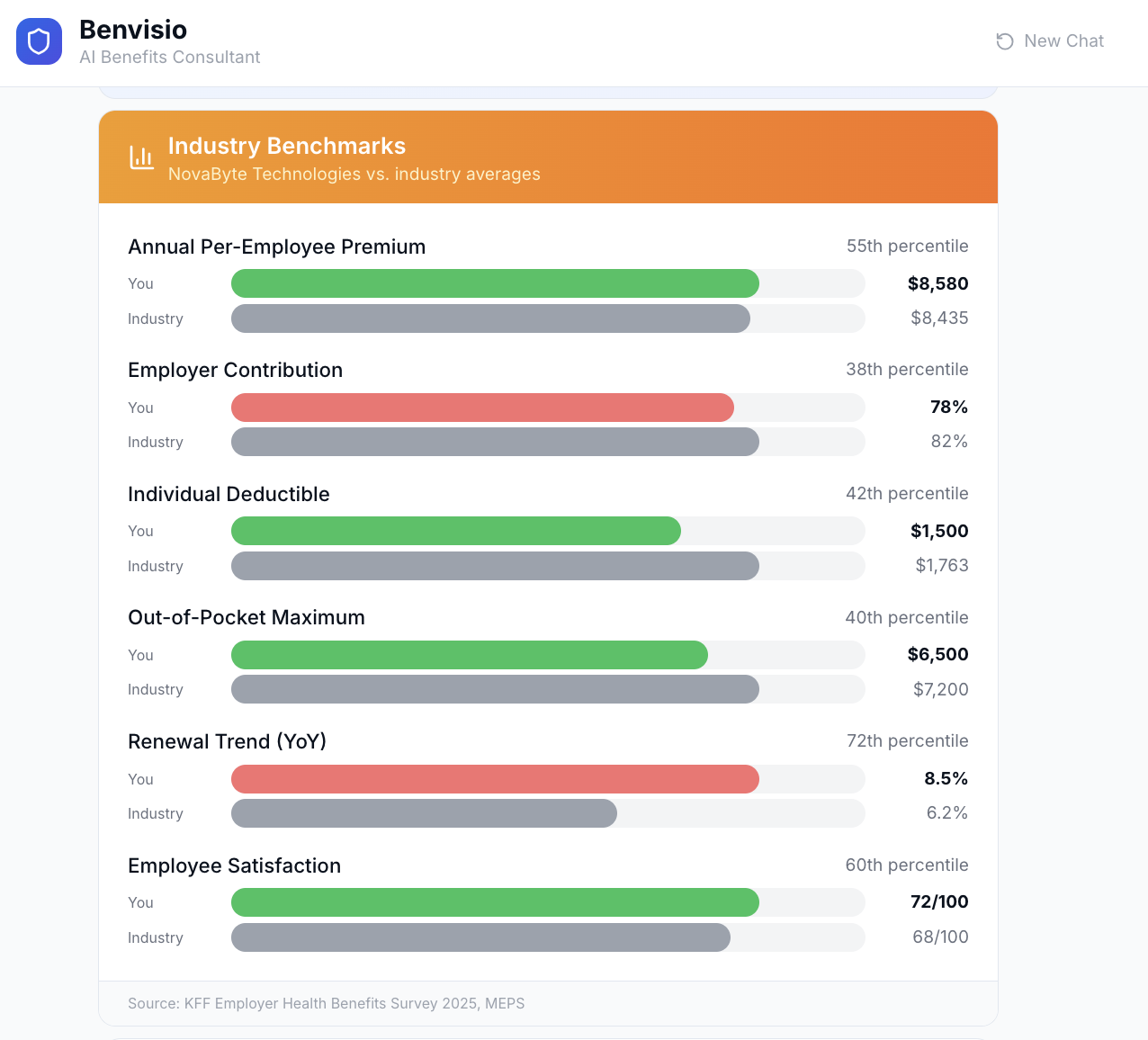
How do your benefits compare to companies your size in your industry? Premium per employee, contribution %, deductible levels, satisfaction scores.
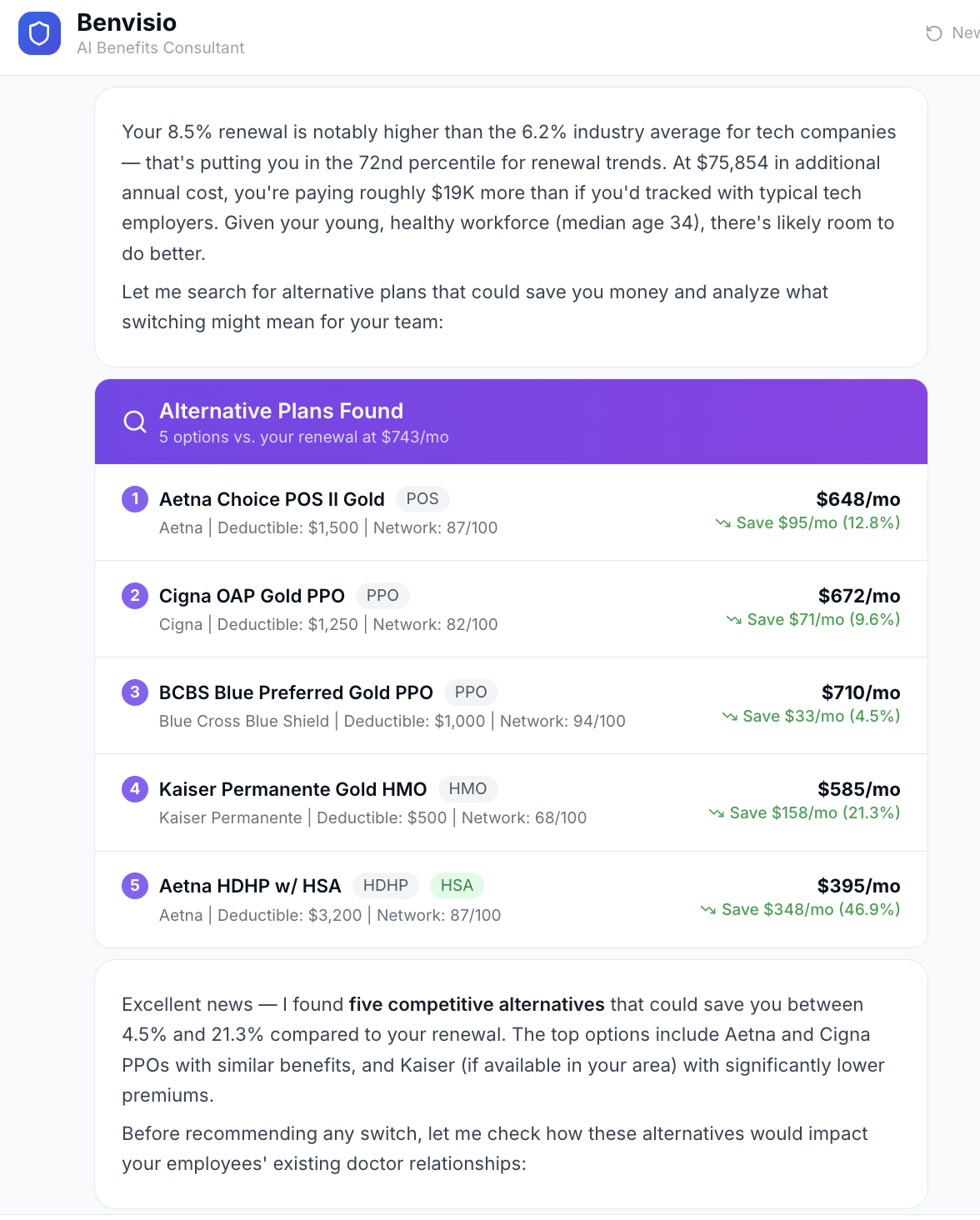
Walk into carrier meetings with data, not hope. Know your market position, have alternatives ready, and negotiate from strength.
Fully insured, self-funded, level-funded, ICHRA, bundled, best-of-breed — Benvisio models every strategy so you can make confident decisions.

Benefits aren't a once-a-year decision. Benvisio monitors plan performance and surfaces savings opportunities throughout the year.
“For the first time, I could show our CFO exactly where our $2M benefits spend was going — and present three concrete strategies to save 15%. The board approved changes in one meeting.”
How It Works
Upload your census, claims data, plan documents, or connect to your benefits admin platform. Benvisio ingests and structures everything automatically.
Have a natural conversation with your AI benefits consultant. Ask about renewals, compare alternatives, model funding strategies — all in plain English.
Rich visual reports, side-by-side comparisons, employee impact analysis, and clear recommendations. Export board-ready presentations in one click.
Platform
A comprehensive suite of AI-powered tools designed for the complexity of employer health benefits.
Early Access Program
Join forward-thinking brokers and HR leaders who are already using AI to deliver better outcomes.
Join 50+ organizations in our early access program. No credit card required.